Adult Acquired Flat Foot
What is it?
The tendon of the tibialis posterior muscle becomes inflamed around the ankle and eventually stops working. The tendon is important to support the arch of the foot and allow normal walking.
What are the symptoms?
Pain and swelling around the inside aspect of the ankle initially. Later, the arch of the foot may fall (foot becomes flat), this change leads to walking to become difficult and painful, as well as standing for long periods. As the flat foot becomes established, pain may progress to the outer part of the ankle. Eventually, arthritis may develop.
What causes it?
There are a number of theories as to why the tendon becomes inflamed and stops working. It may be related to the poor blood supply within the tendon. Increasing age, inflammatory arthritis, diabetes and obesity have been found to be causes.
Who is affected?
The commonest group are females over the age of 50, but men and younger adults can also be affected.
How is it diagnosed?
Mr Gordon will take a thorough history and examine you and take some X-rays. This is usually sufficient to establish the diagnosis. Sometimes the diagnosis is not clear and an ultrasound or MRI may be necessary.
How is it treated? (summary)
This will depend on the stage of the problem:
Stage I : Tendon stretched, medial ankle pain (instep), especially on walking; Swelling along tendon; Able to stand on tip-toe on one leg . Usually treated with insoles and physiotherapy.
Stage II : (a wide spectrum) Tendon partially torn; More severe pain and swelling; Increased flattening of the foot; Unable to go on tip-toe on single leg. Treated as above, tendon reconstruction (operation) if necessary
Stage III : Heel is ‘fixed’. Treated with the use of insoles (orthoses); A fusion operation of the hind foot may be necessary (subtalar, calcaneo-cuboid, talo-navicular joints)
Stage IV : Accompanying ankle deformity. Surgery to the ankle may also be necessary
How is it treated ? (more detail)
Stage I :
Rest – Refrain from activity that will exacerbate your condition, such as sports or long walks
Ice – Or frozen vegetables, wrapped in a tea towel, for 10 minutes at a time on the swollen or painful area
Elevation – At the level of the heart, whenever you are able
Anti Inflammatories – If you are able to take these, they will reduce the inflammation and pain around the tendon. They should be taken for a minimum of 6 weeks.
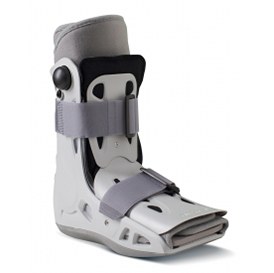
Immobilisation – A removable rigid walking boot may be used for 6 or more weeks to rest the tendon and make walking easier. This should be used whenever you are on your feet, but can be removed at other times including sleeping.
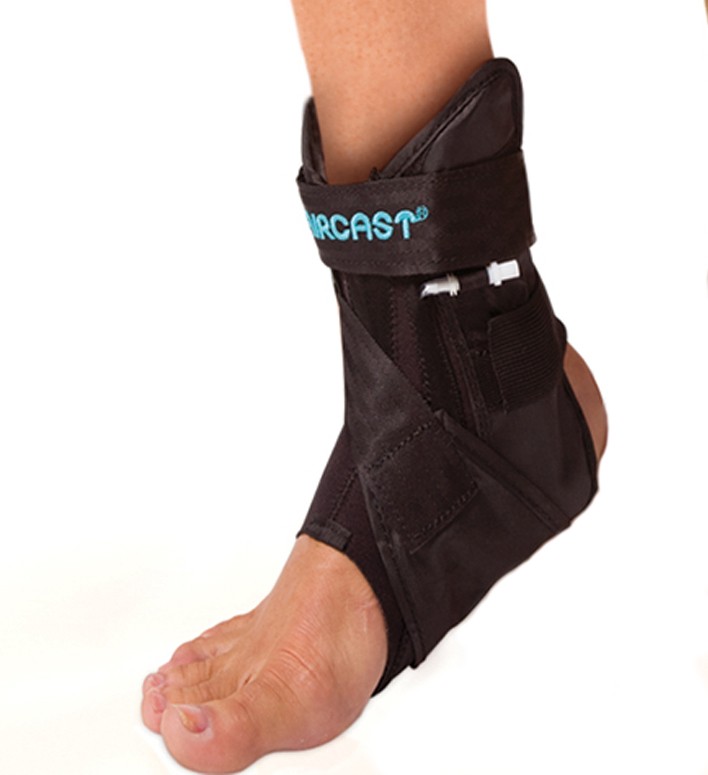
Brace -The AirLift PTTD Brace (made by Aircast) may be used to support the arch (picture below)
Footwear – Flat sturdy lace-up shoes e.g. trainers or boots will help support your foot and provide space for orthoses (insoles).
Orthoses (insoles) – These reduce the strain on the tendon by supporting the arch and reduce pain and inflammation. They may be ‘off the shelf’ or custom made. They should be worn in the rigid walking boot and then in your normal shoe for 6 months.
Physiotherapy – Exercises will increase mobility, strengthen the tendon, stretch your Achilles tendon and reduce pain.
Steroid Injection – Sometimes given under ultra sound guidance.
Shockwave Therapy – An emerging technology, whose benefits are unknown, but is low risk and non invasive
Operation – Rarely needed. The tendon is decompressed and inflamed and torn tissue removed. This can be done through a key hole technique (video below) or ‘open’ surgery
Posterior Tibial Tendonoscopy for Torn and Inflamed Tendon
 |
 |
 |
| AirLift PTTD Brace (made by Aircast) | AirSelect Short Walking Boot by Aircast | Vasyli Red Custom Orthotics – High Density 3/4 length |
Stage 2 :
As for Stage 1 – However, success in avoiding an operation is less likely than for stage 1.
If an operation is not appropriate, the orthosis will need to be used long term
Operation – When non-surgical treatment has failed after approximately 3 months. The abnormal tibialis posterior tendon is removed and a nearby healthy tendon is transferred to replace it. The heel bone (calcaneus) is cut, shifted and fixed, to bring it back under the leg. Stretched ligaments are also reconstructed. Other procedures may also be needed depending on the severity of your deformity. It is performed under a general anaesthetic and nerve block and requires a 1-2 night stay in hospital. You will be in a below knee plaster for 6 weeks with the foot in an inverted position (pointed inward), then a walking boot for 6 more weeks.
The Day After the Operation – You will mobilise using crutches with the help of a physiotherapist, placing only a small amount of weight through the leg (touch weight bearing). Once you are safe to mobilise independently and your pain is controlled, you can then go home, this is usually the day after the operation or the following day.
Weeks 1 – 2 Post Operatively at Home
Strict leg elevation at the level of the chest, for 23 hours a day for 14 days (for pain relief, swelling and wound healing)Regular (3-4 times/day) pain relief (Codeine and Diclofenac)
At 2 weeks, the temporary plaster will be removed and sutures taken out in clinic. A new plaster is applied for a further 4 weeks. At the 6 week stage, the plaster will be removed and you will wear a removable boot and can put all your weight through the leg. Physiotherapy will be started once in the boot.
Potential Surgical Complications
welling – Your foot will remain swollen for up to 1 year after surgery, but will eventually resolve. It is important to elevate your foot as per Mr Gordon’s post operative instructions, to minimise this.
Infection – Despite thorough cleaning before surgery and antibiotics, wound redness and pain may occur, although uncommon. This should be dealt with urgently.
Cutaneous (skin) nerve injury – Near incisions, small nerves can be injured leading to numbness or tingling of the skin, occasionally this is permanent
Prominent metal work – Screws or plates can be prominent under the skin causing irritation. Sometimes these need to be removed with a small operation
Deep Vein Thrombosis (DVT) of Pulmonary Embolus (PE) – You may be given injections of anticoagulant
Stiffness of ankle and surrounding joints – Previous stiffness and 3 months of immobilisation produces stiffness which may not always resolve
Residual or recurrent symptoms and/or deformity – Sometimes the flat foot may not be fully corrected or once corrected, come back, leading to continued problems
Complex Regional Pain Syndrome – Rare
Delayed / non union of heel bone (calcaneus) shift – Rare
Nerve / tendon / blood vessel injury – Rare
When Can I Return To Work After Surgery?
This will depend on the type of work you do:
Sedentary jobs: Return after 2 weeks, if able to maintain foot elevated at level of waist, otherwise 4 weeks off
Standing/walking jobs: Return after 6 weeks
Manual/labouring jobs: Return after 3 months, but may be sooner depending on comfort
When Can I Drive After Surgery?
You need to be able to control the vehicle in an emergency. Can you stamp your foot down on the ground? For left sided surgery and no clutch is required, driving is probably safe at 2 weeks post operatively. For right sided surgery, driving is probably safe at 3 months post operatively, once in a normal shoe. If you are unsure, please ask Mr Gordon. Always notify your insurer of the surgery.
Stage 3 & 4:
These are salvage procedures as arthritis has developed. A joint fusion operation may be necessary to correct the deformity and fuse the bones together to remove pain.
 Call for an Appointment
Call for an Appointment